In the midst of B.C.’s opioid crisis, two Chilliwack nurses are doing their part to get naloxone kits in the hands of anyone who wants them.
“It’s important to get this information out, it really is,” says Sue Griffin, registered nurse at Sto:lo Health Services (SHS). “I have 200 [kits] in my office and they need to get out there.”
She, along with licensed practical nurse, Tanja Tomlinson, is hosting a one-hour free naloxone kit seminar this Sunday which is open to everyone.
The topic is close to both of their hearts. Tomlinson’s father died of an opioid overdose and Griffin encounters the concern on a regular basis through her job as nursing supervisor of community health and home care at Sto:lo Health Services.
The one-hour workshop includes how to spot someone who’s overdosed, what steps to take if someone’s not breathing, hands-on instructions on how to use a naloxone kit, and feedback from the participants.
They use saline instead of naloxone, and oranges as the “muscle tissue” in order to administer the solution. People will practise breaking open glass vials of saline, filling syringes, and then inserting the needles into the oranges.
Sometimes it takes several tries to get it right without spilling the liquid. Some people might not feel comfortable practising in front of strangers and would prefer to do it at home. The nurses will be handing out additional syringes and vials of saline to take home for those reasons.
“This is what we want is for people to actually play with the pieces because then they do feel a little more confident,” she adds.
Regardless of whether you’re able to administer naloxone or not, it’s more necessary to open up the person’s airway and breathe for them until paramedics arrive.
“This is actually more important than the naloxone itself. If you fumble the naloxone, if it can’t get injected or if it get spilled, it’s more important to open up the airway and continue to breathe for them once every five seconds,” says Griffin. “You can still continue to provide oxygen to the brain.”
One dose of naloxone typically lasts 20 to 90 minutes. It replaces the opioid in the body by clasping onto the receptors stronger than the opioid does, but only for a period of time and then the naloxone disintegrates into the body.
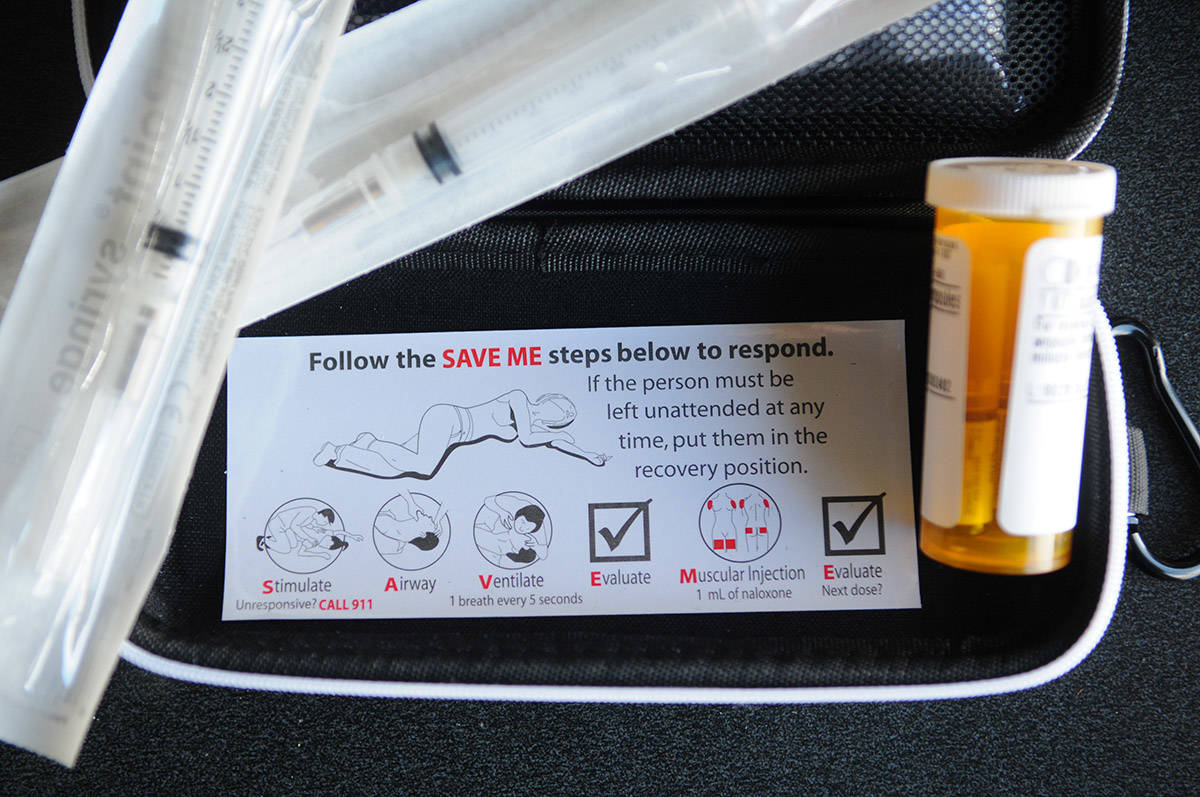
Each kit has three syringes, three vials of naloxone, a pair of latex gloves, airway breathing apparatus and alcohol swabs. The drug is heat-, cold-, and light-sensitive, so it cannot be kept in a vehicle.
Sunday’s naloxone kit seminar is at 1 p.m. at Chilliwack Meeting Space (202-45778 Gaetz St.). It is open to 14 people. To register, email nick@michellebcooper.com.
READ MORE: Decriminalizing drugs the next steps in fighting B.C.’s opioid crisis, doctor says
READ MORE: Agassiz opioid meeting: ‘We have a problem in every town’
If someone wants a naloxone kit, but does not want to take part in the training workshop, Griffin and Tomlinson are happy to help. They’re willing to come to people’s place of work or their home. You can email sue.griffin@stolonation.bc.ca for more.
“There’s no stigma for not doing the training. We don’t want people to feel that I’m going to pry,” she says.
“I don’t want people to think that they have to have the training because it tells you right here what you have to do,” she says pointing to an instructional sticker on the inside of the kit.
As long as the kits are being distributed and people are learning how to use them, that’s what matters most to Griffin and Tomlinson.
@PhotoJennalism
jenna.hauck@theprogress.com
Like us on Facebook and follow us on Twitter.