Fraser Health officials say they're taking new steps to reduce hospital congestion after the release of findings of a review by an independent expert panel.
One of the new methods includes having home care staff based at emergency departments to intercept incoming elderly patients who can be redirected back home and treated there with sufficient home support, according to Marc Pelletier, Fraser's vice-president of clinical operations.
"They can be discharged home with a commitment of home care resources that might be visiting two hours later at that person's home," he said.
Pelletier said that's one of a number of ongoing strategies Fraser is exploring to try to limit the number of people who are admitted to hospital and reduce the average length of time they stay there.
Modest gains in various areas could translate into a huge number of patients across the system, helping cut congestion.
Despite hopes for a silver bullet solution, the Fraser Health Congestion Review Panel said in a report released in June it "couldn't identify any significant gaps" in the region's patient access and flow strategies.
It did suggest potential improvements to explore in several areas.
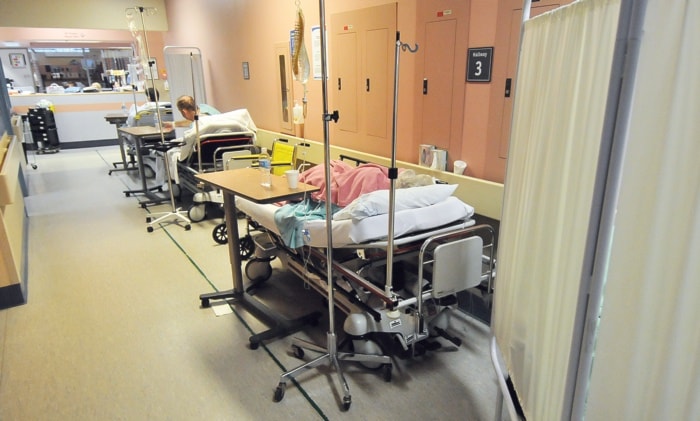
Hospital staff were concerned about the quality of care they could give patients in overflow situations who are routinely treated in hallways, the report said, but many care workers "had a sense of resignation about these conditions as intractable."
The report was released at the same time Health Minister Mike de Jong directed Fraser to pursue measurable improvements in five key areas to reduce hospital congestion within 150 days.
One of the numbers de Jong wants to see drop is the roughly 100 patients across Fraser Health who at any given time are being treated in hallways or other areas not designed for clinical care.
The second target area is a drop in C. difficile infections, where alarmingly high rates of the bacteria-spread illness prompted the health region to send roving "super clean" teams from hospital to hospital earlier this year.
The enhanced cleaning and hand-washing strategies are paying off, Pelletier said.
"We're seeing a reduction in C. difficile to the lowest rates we've seen in a long time."
That should help on the congestion front because patients with hospital-acquired infections tend to stay in hospital longer.
Other minister-set targets include a cut in the average length of patient stay in hospital, an increase in the percentage of admitted ER patients getting a hospital bed within 10 hours; and a goal of treating 90 per cent of broken hip cases within 48 hours.
Pelletier said he isn't concerned the new initiatives might push patients out of hospital too soon, adding staff are "very sensitive to discharging people inappropriately."
The expert panel interviewed more than 500 staff and focused on Surrey Memorial and Royal Columbian hospitals.
Fraser Health last year treated 3.9 per cent more hospital patients and recorded a five per cent increase in inpatient days as well as a 7.3 per cent jump in ER visits.
The 2,200 acute care beds across 12 hospitals are routinely full.
Pelletier noted the new Jim Pattison Outpatient Care and Surgery Centre in Surrey has helped take pressure off Surrey Memorial by becoming the new home for day surgery and most diagnostic tests.
Also on the horizon is the 2014 opening of the new $512-million expansion at Surrey Memorial, adding 150 extra beds.
The province has also committed to a huge redevelopment of Royal Columbian Hospital and expansions or redesigns are also under consideration at Delta, Eagle Ridge, Burnaby and Peace Arch hospitals.