Deaths due to illegal drug overdoses hit staggering heights last year and are on pace to climb 50 per cent higher in 2017.
“It’s going to get a lot worse before it gets better,” said Samantha Ruttan who, like many others in Chilliwack and across the Lower Mainland, has seen the ravages of the current public health emergency that is drug overdoses.
Ruttan is not in social services nor is she a frontline health worker, she owns three gas stations and she’s tired of seeing B.C.’s opioid crisis play out in the bathrooms of her businesses.
“When someone is overdosing it is quite scary,” Ruttan said this week. “You get that flight or fight instinct and you are like a sitting duck if you don’t know what to do.”
Approximately three months ago Ruttan had three separate incidents in bathrooms in the three Shell stations she runs: at Eagle Landing, Cottonwood (Vedder Road and Luckakuck Way) and Chilliwack (Yale Road and Hocking Avenue).
In the Cottonwood incident her staff got a call from the adjacent Tim Hortons that a drug user was heading over. Griffin Security was called but by the time they arrived, a woman had already injected. She then overdosed but was revived with naloxone.
In another instance at the Chilliwack location, a man asked to use the bathroom. They have a policy that it can’t be used for more than 10 minutes after which time staff knocked on the door. He told staff he was fine, then five minutes later 911 was called. The dispatcher told them to open the door and sure enough, the man was overdosing on the floor.
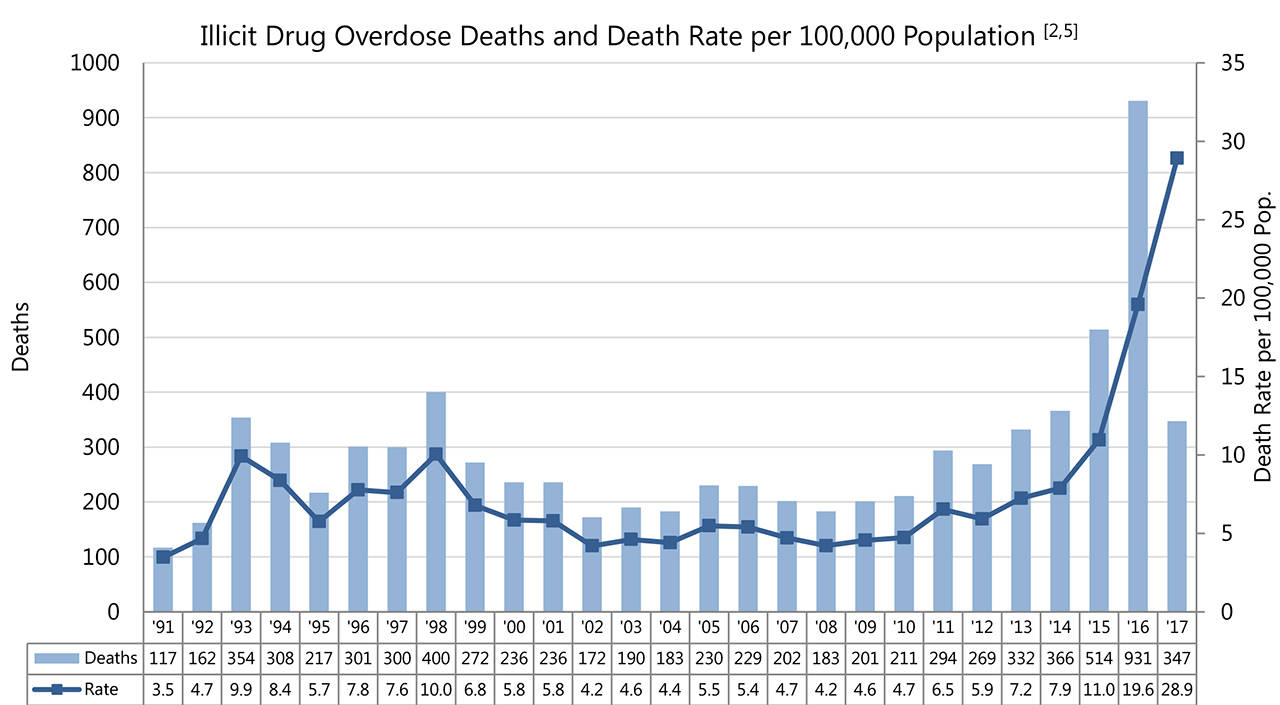
According to the latest numbers from the B.C. Coroners Service, there were 120 illicit drug overdose deaths in March 2017, that’s up 51.9 per cent over March 2016. In the first quarter of 2017, provincewide there were 347 deaths. If that pace continues that would total 1,388 for the year, up 49 per cent over the 931 in 2016.
In Chilliwack, there have been five deaths in the first three months of the year. If that rate continues the city could hit 20. There were nine each in 2016 and in 2015. Provincewide, more than half of the overdose deaths occurred in private residences and 10 per cent occur outside or in vehicles, but more than a third (34.3 per cent) occur in other inside locations such as bathrooms at businesses.
Ruttan said these were shocking incidents, but she wonders how many overdoses go undetected because so few people know the signs.
“You drive around and you see people sleeping all the time, but are they sleeping or are they in medical distress?” she said.
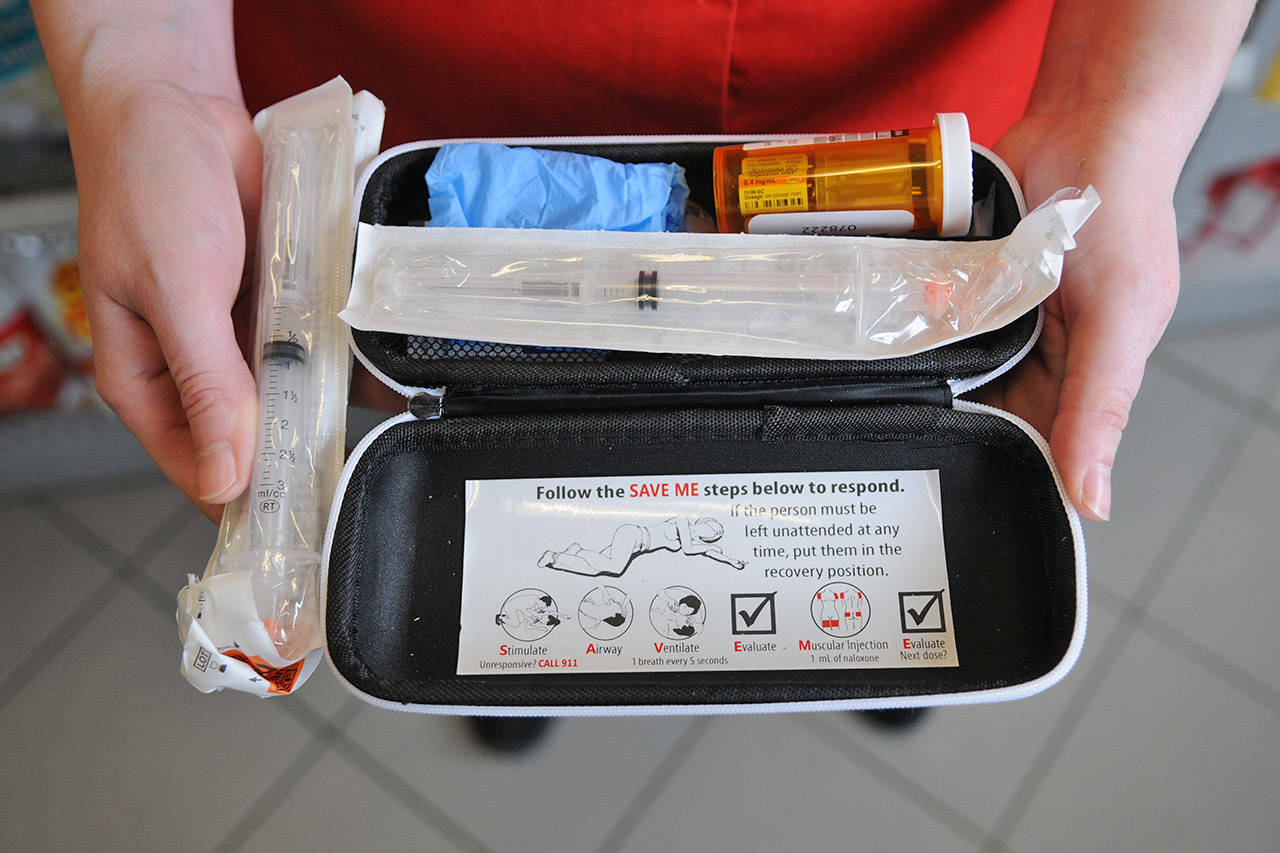
The first thing Ruttan did is put new locks on doors at the two stations that didn’t have them already, but she decided she needed to do more so she contacted Fraser Health. Her request to get naloxone kits and learn how to use them was supported and she and 20 staff went in on May 11 for the training.
“The public health emergency is impacting people and communities across the entire region,” Fraser Health spokesperson Tasleem Juma told The Progress Wednesday. “We are working with all our community partners and that includes private businesses.”
Ruttan said Shell has a policy about calling 911 in such incidents, and she definitely is not ordering her staff to intervene. They have the naloxone kits at the stations now and if someone overdoses, they are to call 911 and if they don’t feel comfortable intervening, they don’t have to.
“But I want them to have the training so they know what it is. I think it is really important that my staff gets trained, not just for Shell but for their personal lives as well,” she said, pointing to the increasing incidents of fentanyl-laced party drugs.
And she recognizes the concerns an employee at a gas station might have dealing with a drug-addicted person in the throes of a medical emergency. In addition to the obvious concern about getting stabbed with a needle, there is more.
“There are a lot of concerns, yes, so for example if you give the Narcan [the brandname for naloxone] they are going to come to and their high is going to be over,” she said. “So they are going to get pissed off, so it’s really important that as soon as you administer it that you back away from them and explain to them what is happening.”
As of April 19, Fraser Health has made Take Home Naloxone (THN) kits available to the general public. The Chilliwack Public Health Unit also offers no-cost training to anyone, and no cost THN kits to those who are eligible. The kits are available for free to anyone who uses illicit substances or has a history, as well as family and friends of users.
The kits are generally not free for private businesses, but they can be purchased at pharmacies. In the case of Ruttan and her Shell stations, Fraser Health and provided her free kits because of the “frequency of overdoses.”
Juma also directs people to find out more at the B.C. Centre for Disease Control’s harm reduction website Toward the Heart.
In Chilliwack and Agassiz, THN kits and training are available at the following locations:
- Chilliwack Public Health Unit – 604-702-4900, 45470 Menholm Rd.
Group or individual training, Monday to Friday: 8:30 a.m. to 4 p.m. Call to confirm staff availability
- Cedarview Clinic – 604-792-1070, 9380 College St.
Individual training, Monday to Thursday. Call for information
- Primary Care Clinic – 604-702-2850, 45600 Menholm Rd. (Chilliwack General Hospital)
Group or individual appointments, Monday to Friday, 9 a.m. to noon and 1 p.m. to 3 p.m. Call to confirm staff availability.
- Riverstone Detox – 604-703-6986, 45600 Menholm Rd.
Seven days per week, 8 a.m. to 4 p.m. Mobile Access available (may be able to provide service to other Fraser East communities). Call for appointment.
- Agassiz Community Health Centre – 604-703-2030, 7040 Cheam Ave.
Group and individual training, Mondays and Fridays, 9 a.m. to 4 p.m. Call for appointment.
- Agassiz Public Health Unit – 604-793-7160, 7243 Pioneer Ave.
Group and individual training, Mondays and Fridays, 1:30 p.m. to 3 p.m. Call for appointment if able.